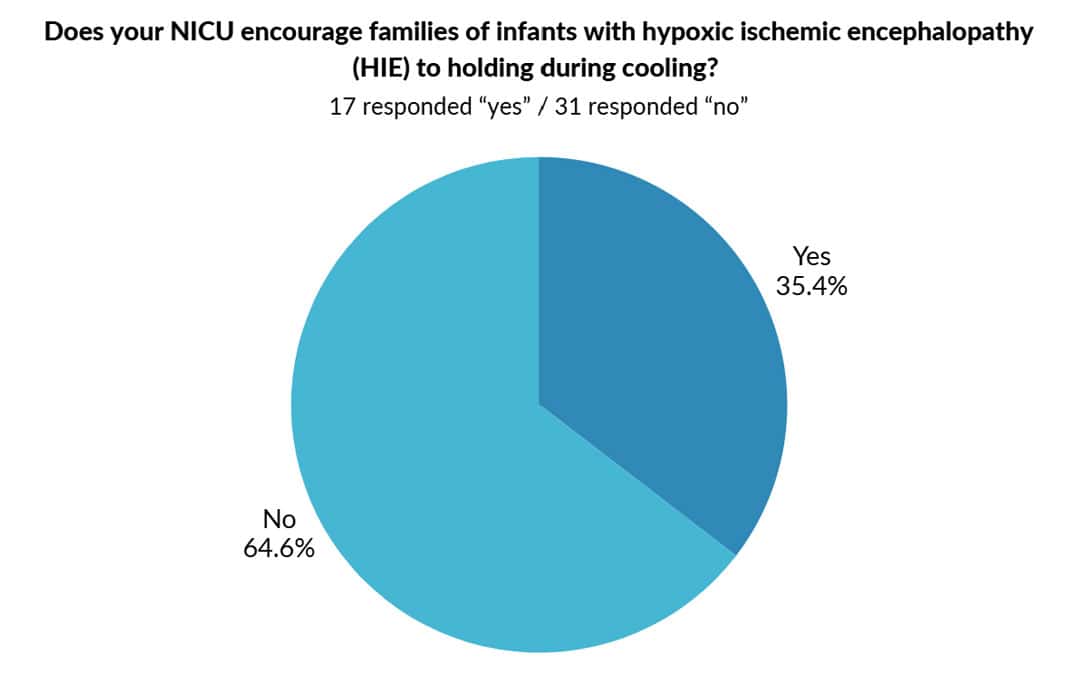
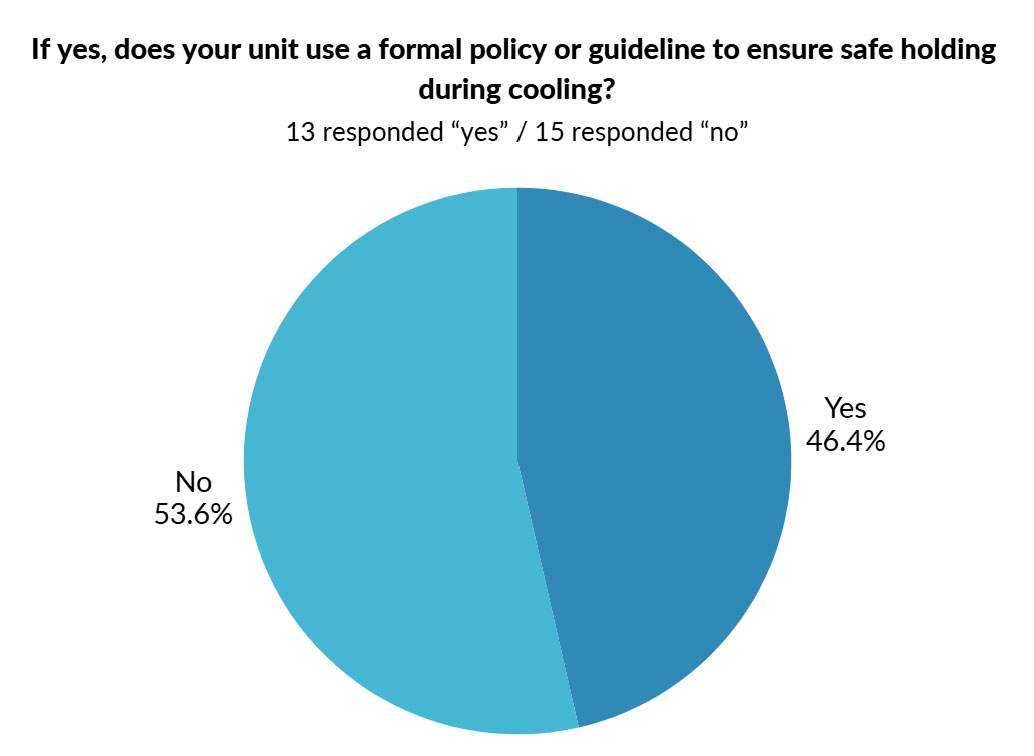
Help us support units seeking to implement holding during cooling for infants with hypoxic ischemic encephalopathy (HIE).
If no, what challenges does your unit face that prevent holding during cooling?
- Provider buy-in
- Lack of information
- [Lack of] aEEG (amplitude-integrated electroencephalography)
- Cultural beliefs, parent’s condition
- Physician resistance
- Not part of our NICU policy
- It varies, case by base. There are situations where there is support to hold during cooling, especially if patient is on minimal respiratory support. The challenges appear to be rooted in the amount of support needed for various organs, aEEG, and overall stability of patient. There has been an increase in allowing holding recently, but not standard.
- We use a cooling mat
- Physician and staff buy-in
- Comfort of providers and staff
- Safety concerns, equipment barriers
- Patient safety issues, challenging transfer to holding, parents’ and healthcare professionals concerns and fears
- We do not do cooling at our facility
- Neonatology buy-in, holding during rewarming has happened
- Probably nurse comfort level as babies tend to have many lines, intubation, aEEG, etc. I personally think we should allow holding!
- Lack of knowledge and expertise
- Our policy states that cooling patients will have a UAC line, that prevents them from being held while line is in place; maintaining low temp
- Possibly educating neonatologists and other medical staff more about this
- Not sure if we have a policy stating that they must be in the isolette
- Nurse time and availability
- Support of holding during active cooling is inconsistent
- Security of other babies and we have specific feeding hours
- We don’t know
- [Lack of] aEEG equipment
- I would love to see a policy or the logistics for maintaining EEG leads and the cooling blanket, etc.
- Team members don’t have enough experience in doing that and are concerned for the infant
- We just have general guidelines not to exceed an hour and to have a pillow under the baby in the cooling wrap to minimize heat transfer. Our less stable babies don’t tend to be held. It doesn’t happen often for this population as they also have CFM needles in, often are intubated, catheterized, and have central lines. But it is possible. I think staff awareness and education of how to go about doing it and become more comfortable are a big part of our barriers, and also just the risk for the sickest who are barely tolerating cooling let alone the amount of movement and stimulation. But the less compromised ones we could do better.
- Don’t have proper equipment to have babies held while being actively cooled
- Logistics of the mattress, stability of baby
- Nursing comfortability; usually many tubes/lines in place
- The severity of the illness
- EKG
- Our unit does not formally initiate cooling, rather we prepare babies for transfer to a tertiary setting. While stabilizing for transport, we do not allow for parental holding (in most cases)
- Staffing with high acuity
- No Techotherm blankets or other available clinical technology to do it safely
- Lack of education/experience doing so safely