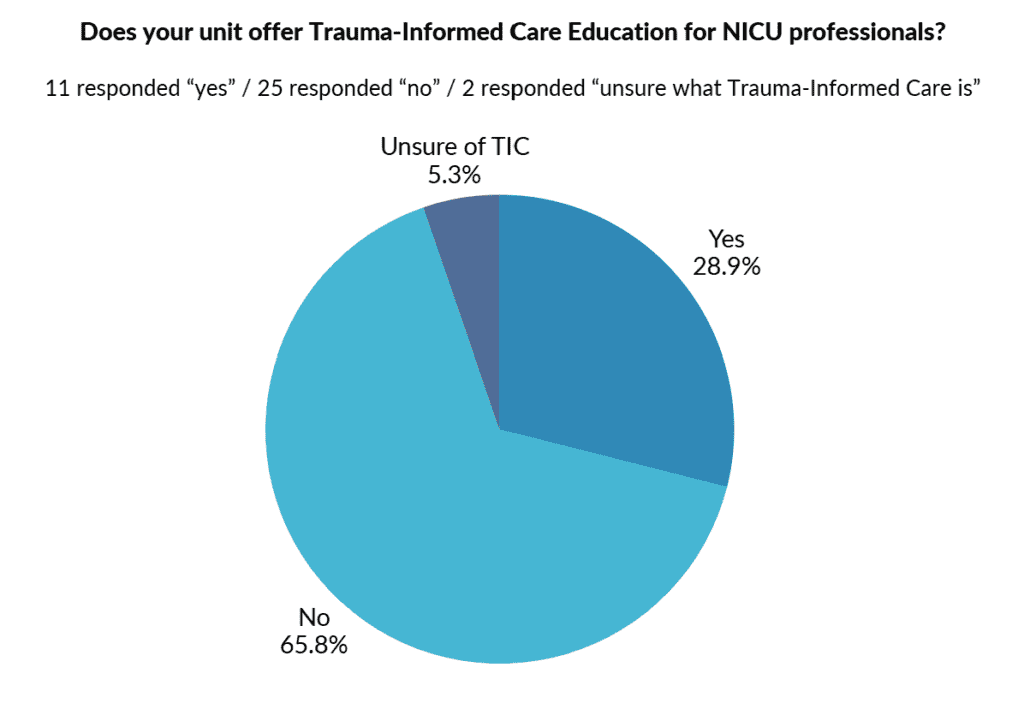
Help us support NICUs working toward implementing Trauma-Informed Care education for NICU professionals.
If yes, please share what you can about your program:
- We have done a brief, one-time offering, summarizing from a conference I attended. It was optional. I would like to offer more.
- I am working at School of Nursing and Midwifery, NICN and Pediatric Department. I recently became familiar with Truma informed care approach when connected with Mary Coughlin and read her bool and attended one her webinar, also in NIDCAP Trainer meetings. In our NICUs, there is no specific program on this topic. Last year I was a scientific director of Nursing international paediatric conference and I invited Mary Coughlin gave a lecture on this topic. I am covering this topic in my NICN classes. I am not sure in our NICUs there is a specific program on this topic. If you have any specific Module, I can work on it and educate by holding workshops for NICUs. I few years ago have lecture used Mary Coughlin book of course this book not available for us just used as online reading and got advantage of it.
- we do FINE and NIDCAP training on our NICU
- Focus of Nursing Conference this year
- SLP/NIDCAP Professional and previous CM/Social Worker completed the Trauma Informed Professional curriculum through Mary Coughlin’s work with Caring Essentials.
- All 3 OTs on our NICU are Trauma Informed Care Professionals through Mary Coughlin’s program. We have provided 50 minute presentations to the pediatric outpatient therapy staff for Unity Point Health hospital systems and the RN’s in our NICU but the attendance was voluntary and turnout was poor.
- Turas eLearning modules, NHS Scotland Trauma Informed Unit, Association for Child and Adolescent Mental Health Special Interest Group on ACEs, EACH – European Association for Children in Hospital and Health campaigns for FCC at all ages of childhood
- System made model. Brought in speaker. Have some staff in a training cohort. Have TIC committee
- Mandatory modules from the health region (adult based content). Education in professional development days and lunch and learns to teach trauma informed care.
- We have multiple decompression sessions after every traumatic event that include out behavioral medicine psychology team. These sessions are for every member of the NICU team. These can be online, in person, or both with the help of Microsoft TEAMs.
- We just recently held a Women’s and Children’s conference that was open to all professionals from these areas. One of the focused topics was Vicarious Trauma. One of our behavioral health psychologists presented on the topic and had a panel of nurses describe a time where they experienced vicarious trauma.
- I provide this education as the RN developmental care specialist, which is included in the NICU developmental care class. The education is included and required for all new NICU RN, PCT, Lactation Consultant, SLP, PT, OT, APP, and RRT staff.
If no, what are your unit’s barriers to implementing Trauma-Informed Care education?
- Our unit got a grant to allow 50 staff of all professions to go through the online TIP certificate program with Mary Coughlin. The nursing educator who led that project moved on almost immediately after it was over, and there is no “leader” to keep it going. I understand not getting another HUGE grant for others to go through the program, but I was under the impression that once we had such a large group, we would then continue the program within the unit ourselves. WHY does nursing leadership make all the difference??? This is coming from a PT who although has been here 20 years, is still considered “ancillary” both from the NICU and my own Rehab Therapies Department who will not give me time to do anything outside of patient care (shhhhhh- don’t tell them I listen to your monthly office hours while I document!).
- not a priority with nursing leadership
- We need resources before we can move forward with TIC
- Always full and working on putting out fires. No persons with trauma informed care and NICU background in our institution
- I believe not enough interest. Need a champion to get it started.
- Recognizing it as a skill
- Education and training opportunities are not available currently. Costs. Covering staff to do any training.
- In my opinion, the barriers are related to budget, lack of support from a leadership and organization level and lack of understanding of the value of the training.
- Our Children’s Hospital received a one-time grant about four years ago to have a cap of 50 employees, mainly nurses apply to receive Trauma Informed Professional training from Caring Essentials (Dr. Mary Coughlin). I received training through this outstanding program. No ongoing NICU-specific offerings are available or covered financially, though I believe trauma-informed training should be integrated into everyone’s work with infants, children and families.
- There is a culture of bullies
- Barriers are very busy wards, unfamiliar with this topic and program and shortage of nurses and high stress they had. I can connect with them and ask them, but I am sure most of them did not hear this term (TIC). May be had some activities align with TIC but did not name it Trauma informed care. Sometimes I am taking my students practicum in NICN and teaching staff too, but unfortunately they are always bust to attend my clinical education class too.
- Small unit that is growing/not sure people have thought about it. I’m trying to advocate for bringing this perspective to the unit.
- Money
- Best way to self educate?
- need resources to develop a program
- Administration is not engaged in trauma informed care. The expense to education all of the NICU staff is not seen as a priority. The unit struggles with family centered care regularly.
- Lack of psychology professionals and knowledge on this subject
- All 3 OTs on our NICU are Trauma Informed Care Professionals through Mary Coughlin’s program. We have provided 50 minute presentations to the pediatric outpatient therapy staff for [our] hospital systems and the RN’s in our NICU but the attendance was voluntary and turnout was poor. Attendance by RN’s was not mandatory. Attempted to write a grant to get more RN’s TIP certified but the unit opted for Engage Grow Thrive education instead.
- It is touched on in our orientation program, but not a full education – time constraints
- Staffing, finances to seek education support
- No, I’m really the only one here that knows about it.
- Reaching the entire staff. Easy to reach the nursing staff than other allied health professionals.
- Funding and resources
- Need education for our educator
- There is so much education that is mandated by our employer it is hard to add anything additional.
- Staff resistance
- I am not sure if there is additional information on this as I am a new team mate and new manager.
- It’s not a leadership priority
- Few trauma-informed clinicians that I’m aware of, lack of training
- Money & time